The 5 Most Common Private Practice Compliance Blunders and How to Stop Making Them

Optimize your revenue cycle and strengthen your billing department by building a diversified payer mix, negotiating smarter contracts, improving documentation, and tracking key metrics to stay cash-flow positive.

When beginning revenue cycle management, we need to talk about what type of payor sources you may be looking at. The most common payor sources that private practices look at are commercial health insurance payers. That's your Blue Cross, United Healthcare, Health Net, the list goes on.
We've also got Medicare, Medicaid, workers compensation, personal injury, government contracts, staffing contracts, grant funding if you're a 501c3, private pay, of course, and more. You've got employer funding, FSA, HSA, and all different ways to diversify your payer mix.
We want to diversify your payer mix because you don't want to put all your apples in one basket. Different payers have different pros and cons. The key is to diversify it based on cashflow margin, client retention, et cetera.
You want 60% of that payer mix paying you 100% within 30 days or less. It's so important. And when I say 30 days or less, that's 30 days from the date of service. So as you build your billing department, it's essential to get those claims in on time.
Again, you want 60% of your payers paying you in 30 days or less.
One of the questions I often get is Brandon, how do I get these commercial contracts? I'm interested in playing in the insurance game, and where do I begin?
If you're going to do Medicare, the critical areas for going after your commercial contracts are as follows. I want you to identify, first and foremost, what contracts are you interested in?
Back in the day when I was in California, my initial contract with Blue Cross actually required us to go through a network called PTPN. That's not the case anymore and you'll want to research lots of networks. As always, you can call me if you need a list of those networks.
I want you to also think about identifying your credentialing needs. When you're partnering with these contracting bodies, there are several credentialing requirements, whether it be a CA or direct credentialing with the insurance company. Start your research now.
You want to submit a formal or informal RFP request for proposal. Now, whenever you write an RFP, it's imperative that you target what that payer source is looking for.
Typically, the payer source is looking for:
I want you to make sure that you have your billing department locked down, whether in-house or third party. You have to be ready and know that your documentation policies are together.
Do you have clinical documentation set forth that's going to align with what that medical insurance is looking for?
When you're dealing with medical insurance, it's vital that you identify the goals of your clients, in terms of how it relates to the payer source. It's so crucial that all your goals are targeting the medical necessity of the patient.
Suppose you're a physical therapist or a mental health professional working on mental health goals related to the medical necessity and the client's mental health. In that case, all of these areas are essential in your documentation. Your documentation and your clinical outcomes are how you justify them paying you for your services.
The other day I was on the phone with a private practice in Houston, Texas. She's been in business for 18 years, and she asked me, how do I negotiate with these commercial payer sources?
And I said, well, have you ever had a raise?
She said in 18 years, she had never asked for a rate increase.
And I said, have they ever given you one?
And she said, no, they've only taken money away from me.
Well, if you don't ask, they assume that you're satisfied with your rates. So there are several keys to negotiating with payer sources. You have to show the following data:
Now, I always say your payer sources are focused on money, as well as satisfying the necessities of their clientele. Here's an example:
Hey, Blue Cross. Suppose I can get $25 more per visit. In that case, I can deliver a full 60-minute visit where I'm going to actually increase the clinical outcomes so that I can discharge your clients sooner.
So rather than you paying for 18 visits, I'll get it done in 12, and in the long run, you're going to save money, and you're going to have happier clients.
That's how you negotiate a payer source to align with their goals. Provide metrics and a finite period of time that you're going to accomplish successful actions for them. It's a win-win for all because you are growing your margin to deliver a higher quality service.
The client wins because they're getting better services and reaching their outcomes faster. The payer source wins because the big picture financial investment gets better for them. You have to think about each party and what they're trying to accomplish as you attack the negotiation.
It's so essential for you to think about this. No money, no honey, as I always say. You have to understand what the driving forces are for the payer source. You have to understand they're looking to save money. So you need to make a claim that what you're exchanging with them is in abundance. That's important.

Cash positive is not just cash pay. It could be other another payer mix that pays you in that 30 days or less. So the first thing to do is you want to identify your niche. What separates you? How do you differentiate?
I have a feeding practice where we're among the few specializing in working with infants who have swallowing disorders. That's a niche.
For example - I'm going to offer a telehealth service at no additional cost. The patient receives a home exercise program with coaching delivered to them once a month as part of our contract.
I want you to build a program with mailbox money. Mailbox money is money that's coming in that doesn't take manpower.
Create a program where 30 days after a discharge, for a $99 a month fee, they can access your gym, equipment, home exercise programs, and videos that you've delivered for them to reference. All of those things are mailbox money.
I want you to create, execute, and empower the customer experience. How do you focus on rehabilitation and putting resources together to prevent future challenges that they may face? Maybe you're incorporating some diet strategies. Maybe you're including some fitness. There are so many different ways to embrace preventative health in today's environment by incorporating preventive measures that lead them to success.
Let's make those metrics matter. Let's manage your market retention. I want you to evaluate how long people stay within your program and how you have transitional care that supports them throughout their lives.
How do we think outside the box? How do we relate with, not just this next generation of millennials, but also other generations? Innovation is key.
Problems ranging from costs to medical errors beg for solutions, and indeed, huge investments have been made in innovation. But too many efforts fail. To find out why, we must break down the problem, look at the different types of innovation, and examine the forces that affect them.
And this is really important. Whether you outsource your billing department or keeping it in-house, you need to identify your needs based on scalability, the complexity of payer mix, and fixed overhead versus variable overhead costs.
What can you afford?
So when you're outsourcing a billing department, it's typically a variable cost, meaning that you're paying a fee anywhere from 6% to 8% of all collectible income. When you're small, I actually recommend the variable of outsourcing, as long as you have measures to hold that third party company accountable.
I also want you to think about liability and control. We're going to talk about this next, but something to think about is if you give the keys to your billing department away, do you have control there?
Whether it's a third-party provider or in-house, the ability to manage and ensure accountability is critical. So if you're one of these clinicians that you're just like, Brandon, I don't know what to do. I don't know billing.
Okay, well, there are several key metrics that you can hold that billing department accountable to, and we're going to talk about that in a minute.
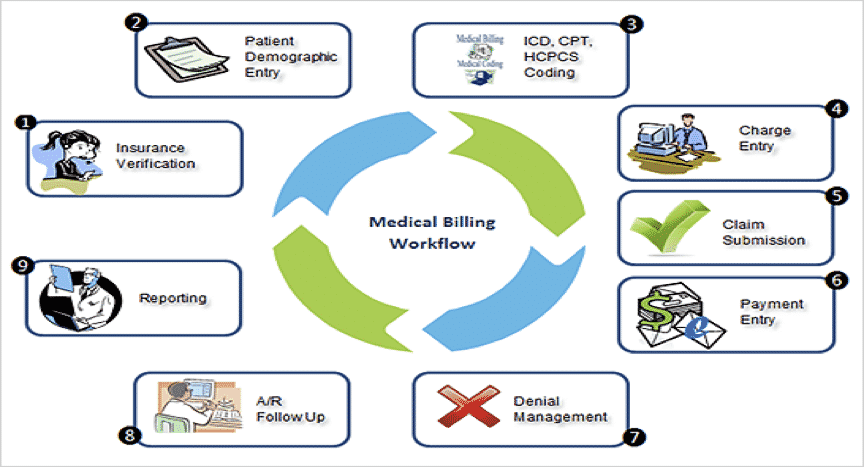
I want you to understand the diagram of what a billing department looks like. It's imperative. Step one, you've got to verify the insurance.
I always say verify the benefits. If they're coming through insurance, verify their benefits before you bring them in. More often than not, I find that clinics bring the client in, do the evaluation, and then start the billing process.
Do you know how hard it is to collect from someone when they're expecting to come in and only pay $5, $10, even $40? So if they're looking to access their insurance, verify their benefits, or have them verify their benefits in advance and provide you the information.
Then I want you to enter the patient demographic info, hopefully into your medical EMR system, your electronic medical records system. We have to make sure the coding is correct. Get your ICD tens, understand your treatment codes that you're utilizing.
Then you have someone charge entry. Usually, that's going to be in-house. Your front desk person will actually enter the charges based on how the clinician delivers the service, or the clinician may even enter it. Then we submit the claim, and that's where I'll find third-party vendors usually get involved.
They double-check the charge entry, submit the claim, and enter any payments received. They also troubleshoot the denials. What happened? Do they need more medical necessity proof? Do they need to see records?
There are accounts receivables that need to be followed up on to make sure we get paid both on the insurance or commercial payer source side, as well as the client-side.
In your billing department, I want you to paint realistic expectation to your clients, so the risk doesn't fall on the provider but instead falls on the client. That's so important. I have this rule of thumb in life, and it's called under-promise over-deliver.
Paint the expectation that insurance won't cover it. Paint the expectation that if within 60 days, if it doesn't get paid, the client will be held responsible. Start to look at those pieces.
Make sure anything that you're holding the client accountable for aligns with your insurance contracts. I always say when you're negotiating an insurance contract, make sure that you're negotiating because an insurance contract is always written on behalf of the insurance company.
Sometimes you need a third party person to look at those contracts, to give you feedback, and to understand how to negotiate that contract to your favor. Know that there are resources out there that can help you with that.
Wellness Works Management Partners has a team of people that support clinics just like you, making sure that you're signing quality contracts.

I see it all the time. I'm sure you've seen it. They literally, I don't know billing. Here's my keys. You do it. Just get me paid.
Please don't do it.
Ultimately, I've never seen a practice give away the keys to the castle and not have significant issues in the AR department. So even though you may outsource things, I want you to hold them accountable. I want you to measure your reports and metrics, understand what's outstanding to get paid, and hold them accountable.
I see it all the time. I walk into a billing department. The first thing I do is I ask the owner, can I look in the drawers of your billing department?
And they say, well, why?
Because I'm going to know how chaotic that department is based on the organization of those drawers.
And they go, be our guests.
Usually, I walk in, and I take out a stack of papers. And what I find is months and months and months of claims that people have kind of brushed to the side. I'm going to get to them. I'm going to get to them.
Nope.
You need organization for your claims department. So essential. An infrastructure, systems, accountability; Nothing should be in your drawers. I repeat, nothing should be in your drawers.
I've seen this in my mother-in-law's practice. Back in the day, I remember coming in, and I went to our finance department, and I said, what's our longest outstanding that we haven't gotten paid.
And she said, Oh, we have some claims, just a couple, but we have some that are over a year.
I said, what? And I said, what are their bills?
And she said, Oh, around $5,500.
I said, no one in their right mind. When I come to those patients and say, I need $5,500, they're going to be like, no.
You need to have your transparency in place, and I never let an AR exceed $500 without a sign-off from the client. Never. Do not let your AR on a client exceed $500 without permission from a client.
This client in Houston that I was speaking with, unfortunately, they signed awful contracts.
I said, why did you sign the contract?
And they said, because I needed the patient volume, Brandon, you don't understand.
I understand that you basically just paid for those clients to get services because you lost money on every visit. I can bring in 300 new clients a day for you, If you want to give your services for free. Even more if you're going to take Medicaid. In some places, you can get lots and lots of clients just rolling down your doorstep.
The problem is you're not going to get paid in many cases for sometimes six months, nine months, a year, or even at all. Don't sign the bad contract. Out create them. The easy route is to say, I'm taking a contract that's just a wealth of leads. I would rather you invest in marketing than a bad contract that funnels clients
I see it all the time. I ask questions. I get your eyes rolling to the back of your head. Confusion, confusion, a little bit more confusion, thus impacting the evaluation of the private practice condition.
A great example of this is billed charges versus contracted charges. For those of you who are playing in the insurance game, they understand that you create a fee schedule based on bill charges because some insurances just pay you a percentage of those billed charges, but your bill charges don't equal what you're expecting to get paid.
Sometimes I inflate my payer expense, my pay list, because I want to get 80% of the highest rate. I'm charging $225, but then you have contracted rates at $75. So you have to make sure you're evaluating the appropriate metrics. Don't evaluate your bill charges, evaluate your contracted rates, and what you anticipate getting paid.
Ensure your private practice owner reviews key billing metrics weekly, inclusive of what's going on in your aging report.
Jump on it sooner than later.
I don't want you to be overwhelmed by anything I'm sharing. I know I spit out a lot of information. These things are broken down in so many places of mine, and I have many more free resources to share.
If you have a question, reach out to me. For those who know me, I respond right away. If you would like a personalized approach, you have nothing to lose. Sign up for a free 30-minute strategy session. Anyone who's done it knows it's not a sales pitch. It's my way of giving back to the industry, to my listeners, to my community.
And yes, that strategy session is hundred percent free. So you get instant value.
You remember I said $500? Have that cap the first visit in. I want them to understand their cap. You have $500 that I put on account for you while I bill your insurance. When we exceed $500, you're going to have an important decision to make. Still, I want you to understand you're responsible for this $500 regardless if the insurance pays for it.
Put the risk on that.
I want you to incentivize both the patients and your employees. Create the buy-in again. Creative compensation to your employees, but then on the payer mix, maybe you actually incentivize your customers.
Hey, I'm going to offer a discount. I do this all the time. Buy 20 coaching sessions with me, and I'll give you a discount. Buy 20 visits with you, provide them with a discount. Maybe it's 10 visits. Collect the money upfront. Have it so that you're cash flow positive.
A practice management and electronic medical record system is a key to not just your metrics, but to electronic claim submissions, real-time claim info, having a patient portal where patients can access their charts.
Get your plan started. Let's make it happen. Let's create the practice you want it to be. Let's do it now, and let's do it together.
Don't forget to sign up for a free 30-minute video consult. We will make it happen. We will push you to the finish line. We can thrive, not just survive.